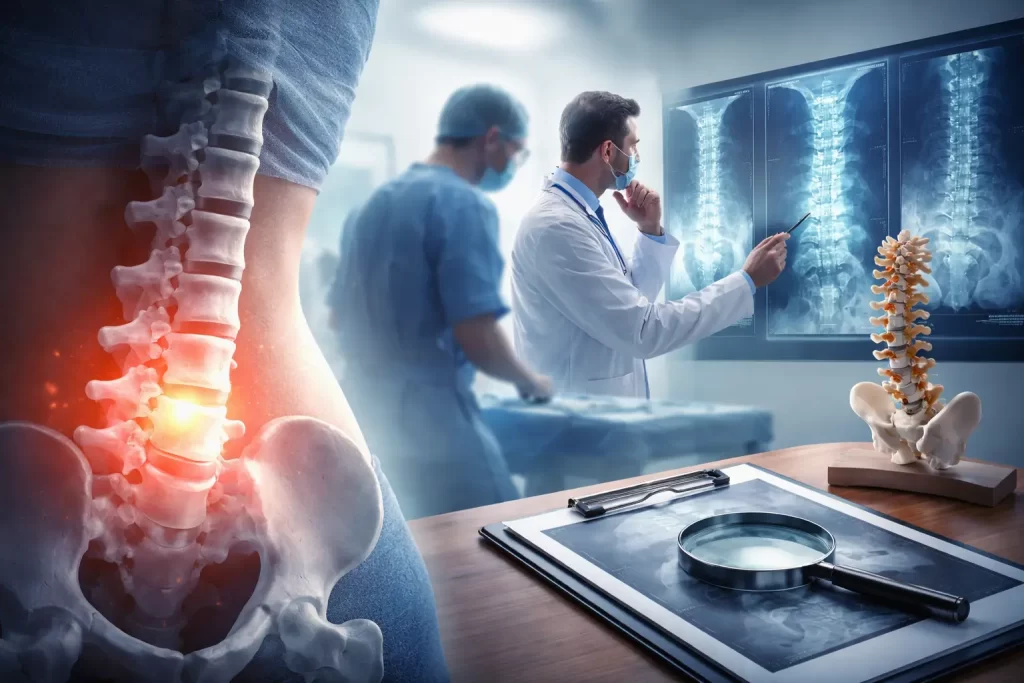
Choosing to undergo major spine surgery is a life-altering decision. While surgery is often framed as the final “fix” for chronic pain, clinical reality is more nuanced. For many, the road to recovery isn’t found under a scalpel, but through a deeper understanding of the spine’s complex biology.
At the Indo British Advanced Pain Clinic, we leverage 25 years of international expertise to provide patients with the transparent truth. Before you “go under the knife,” here is why pausing for an expert second opinion is a vital safety step.
1. The "Success" Illusion: Instant Relief vs. Long-Term Failure
Many patients experience “the honeymoon phase”—immediate relief after surgery followed by a return of pain months or years later. This is frequently driven by Adjacent Segment Disease (ASD). When a segment of the spine is fused (immobilized), the levels above and below must compensate, bearing extraordinary mechanical stress.
Failed Back Surgery Syndrome (FBSS): Statistics show that 10% to 40%of spine surgeries result in persistent or recurrent pain. This is a big failure rate for an irreversible spinal surgical procedure.
The Satisfaction Gap: In long-term evaluations, patient satisfaction can plummet from 80% in the first year to just 22% after several years as secondary issues arise after 2-20 years after surgery.
2. The Metalwork Burden: Biomechanics and Biocorrosion
Implanting screws, rods, and cages introduces a “mechanical intruder” into a flexible biological system. Even with perfect surgical execution, hardware is subject to the laws of physics and chemistry.
| Complication | Estimated Incidence | Impact |
|---|---|---|
| Hardware Failure | 1% – 11.2% | Screw breakage or rod fatigue necessitating revision. |
| Migration/Loosening | ~22.5% | Screws "backing out" or loosening, leading to instability. |
| Biocorrosion (Metallosis) | Variable | Leakage of metal ions causing inflammation and bone loss. |
A second opinion can help determine if your bone density (osteoporosis) or lifestyle makes you a high-risk candidate for these mechanical failures.
3. The Diagnostic Gap: Why MRIs Can Be Deceptive
A common pitfall in spine care is “treating the image, not the patient.” Research indicates that 85% of imaging tests do not accurately identify the functional root of back pain.
- The “False Lead”:Many asymptomatic people (those with zero pain) have disc bulges or “wear and tear” on their MRIs.
- The Functional Root:Often, the real pain generator is a weak muscle group, an inflamed facet joint, or a ligamentous issue that an MRI cannot “feel.”
4. Risks of "Minor" Procedures
Even non-surgical interventions like epidural steroid injections require extreme precision. While generally safe, traditional techniques without advanced guidance can lead to :
- Arachnoiditis: A rare but devastating inflammation of the spinal nerves.
- Epidural Abscesses: Serious infections, particularly in immunocompromised patients.
- Nerve Trauma: Permanent numbness or motor loss due to needle placement or neurotoxicity.
5. When Surgery IS Necessary (and When It’s Not)
Surgery remains a gold standard for specific, urgent conditions. A second opinion helps distinguish between elective surgery and emergency surgery.
- Clear Indicators for Surgery:Nerve compression with muscle wasting, spinal instability (spondylolisthesis), tumors, or loss of bowel/bladder control.
- Indicators for Minimally Invasive Care:Chronic “achy” back pain, discogenic pain without weakness, and facet joint syndrome.
- The Second Opinion Advantage: An interventional pain specialist can use diagnostic nerve blocks to “test” the pain source before any permanent changes are made to your spinal anatomy.
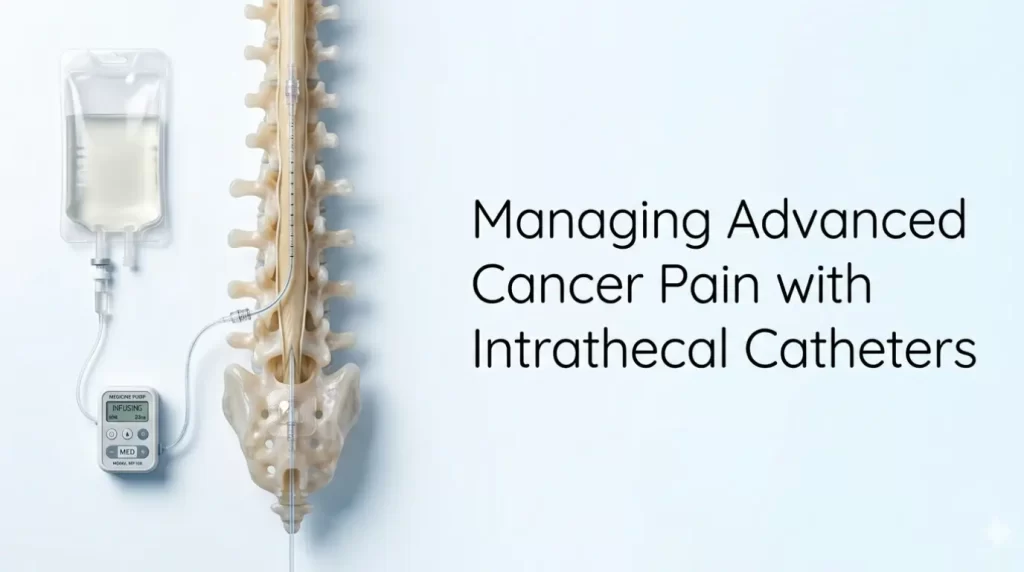
6. Modern Alternatives: The Non-Surgical Pathway
International guidelines now prioritize a “multimodal” approach. Before committing to fusion, consider these minimally invasive options:
- Radiofrequency Ablation (RFA):“Disconnecting” pain signals from arthritic joints.
- Disc Preservation with Ozone nucleolysis, Biaculoplasty or laser decompression.
- Epiduroscopy and Epidural Adhesiolysis for post-surgical refractory pain due to scarring and adhesions.
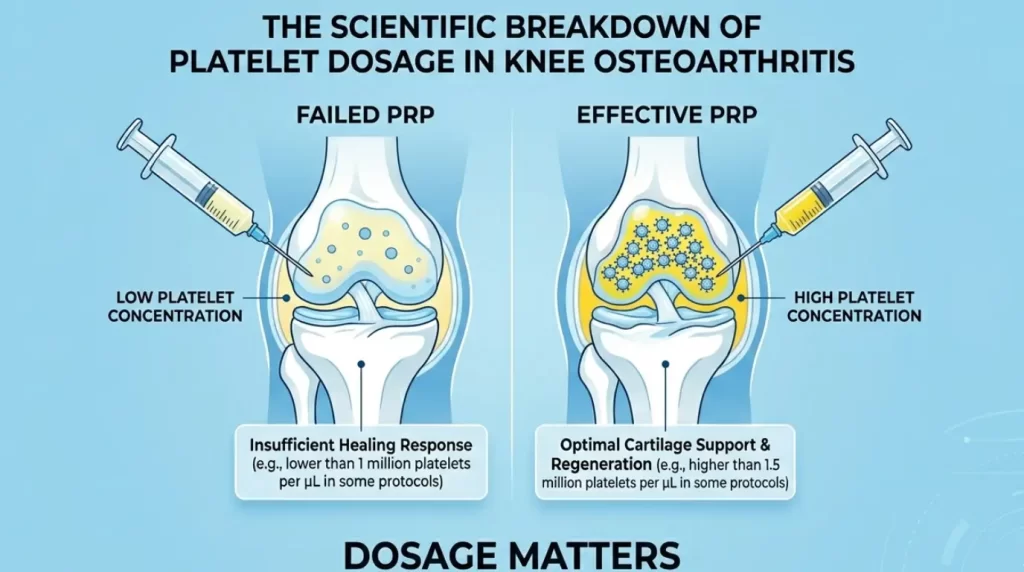
- Regenerative Medicine:Using the body’s own healing factors to repair disc or ligament tears.
- Neuromodulation: Advanced technology to interrupt pain signals before they reach the brain.
Summary: Why Ask for a Second Opinion?
Seeking a second opinion before choosing an aggressive surgical path isn’t a sign of distrust; it is a hallmark of an informed patient. It reduces the risk of:
- Unnecessary multi-level fusions.
- Keyhole surgeries (Endoscopic discectomy)
- Failed Back Surgery Syndrome (FBSS).
- Long-term hardware complications.
If you are being told surgery is your “only option” or feel rushed into a decision, it is time to seek a second perspective rooted in functional recovery.
At Indo British Advanced Pain Clinics, our role in second‑opinion consultations is to review your diagnosis, scans and previous treatments, explain the true risks and benefits in simple language; and help you understand all available non‑surgical, minimally invasive and surgical options. The final decision is always yours—but it should be made with complete, unbiased information, not pressure.
Start Your Journey to a Pain-Free Life Today
Join over 32,000 happy patients who have found relief at Indo British Advanced Pain Clinic.
Locations: Banjara Hills and Madeenaguda, Hyderabad.
Helpline: 9807 55 6789.
Book your consultation with our experts today and discover the freedom of movement without surgery!
Academic References & Data Sources
- FBSS Prevalence:Baber, Z., & Erdek, M. A. (2016). Failed back surgery syndrome: current perspectives. Journal of Pain Research, 9, 147– [Meta-analysis].
- Adjacent Segment Disease (ASD):Hilibrand, A. S., & Robbins, M. (2004). Adjacent segment degeneration and adjacent segment disease: the consequences of spinal fusion? The Spine Journal, 4(6), S190-S194. [Systematic Review].
- Hardware Failure Rates:Galbusera, F., et al. (2015). Rigid fixation and adaptive remodeling: how much implant is too much? European Spine Journal. [Biomechanical Study].
- MRI Accuracy & Asymptomatic Findings:Brinjikji, W., et al. (2015). Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. American Journal of Neuroradiology, 36(4), 811-816. [Systematic Review].
- Re-operation Rates:Martin, B. I., et al. (2007). Reoperation rates following lumbar spine surgery and association with specialist type. Spine, 32(3), 375-380. [National Registry Data].
- Complications of Injections:Epstein, N. E. (2013). The risks of epidural steroid injections: a sensible strategy. Surgical Neurology International. [Review of Clinical Outcomes].
- Evidence-Based Guidelines:Qaseem, A., et al. (2017). Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians. Annals of Internal Medicine. [Clinical Guideline].
- Hardware Loosening:Zou, D., et al. (2020). Pedicle screw loosening in the lumbar spine: a systematic review and meta-analysis. Journal of Orthopaedic Surgery and Research. [Meta-analysis].